In the realm of orthopedic surgery, effective fracture repair remains a significant challenge. The Humeral Interlocking Nail is a vital tool. It has gained popularity for its unique ability to stabilize complex humeral fractures. This technique promotes healing while preserving shoulder function.
Surgeons must choose the right methods for different cases. Various techniques exist, and each presents unique advantages and limitations. A careful assessment of fracture type, patient health, and desired outcomes is crucial for success. Yet, many face challenges adapting to advanced materials and techniques. This complexity often leads to questioning best practices.
Moreover, the learning curve involved in using the Humeral Interlocking Nail can be steep. New surgeons may feel overwhelmed by the intricacies of the procedure. Reflecting on techniques and outcomes helps refine skills. Ultimately, embracing both successes and shortcomings can lead to an enhanced understanding of effective fracture repair methodologies.
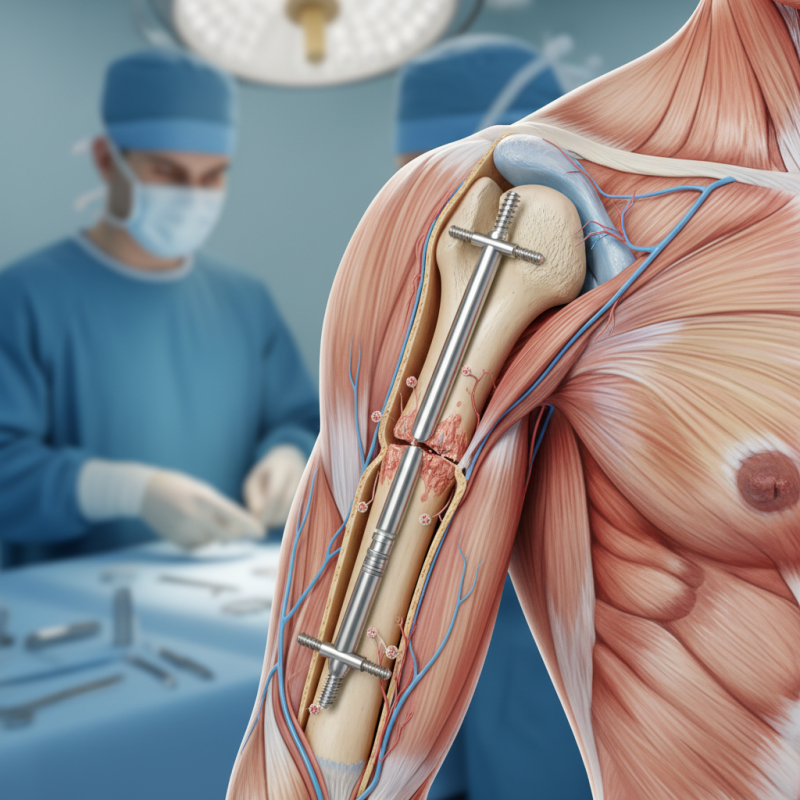
Humeral fractures are common injuries. They often arise from falls or accidents. The humerus, a long bone in the upper arm, can break in various ways. Understanding the types of fractures helps in choosing the right treatment. Some fractures involve the middle of the bone, while others occur near the shoulder or elbow.
Treatment options vary based on the fracture type and location. Surgical methods like interlocking nail techniques provide stability and promote healing. However, these procedures are not without risks. Complications such as infection, poor alignment, or nerve damage can occur. Surgeons must assess the injury carefully. They often use imaging to determine the best approach. Recovery can take time, and rehabilitation is crucial.
Patients should understand their treatment options fully. Communication with healthcare providers is essential. Some might not see improvement as expected. A proactive approach to recovery can lead to better outcomes. Life after a fracture can be challenging, but awareness of potential issues is vital.
Interlocking nails have become a staple in orthopedic surgery. These devices provide stability for fractured humeral bones. Their design allows for effective fixation, promoting healing. Surgeons often face challenges when choosing the right technique.
One common method involves anterograde insertion. This technique can be effective but may require precise alignment. Surgeons sometimes struggle with achieving the perfect angle. Misalignment can lead to complications. In some cases, using a retrograde approach may be beneficial. This method can provide better access but comes with its own set of challenges.
Surgeons must assess each case carefully. Not every technique will suit every patient. Factors like fracture type and patient health play a critical role. It’s essential to remain open to learning from each procedure. The effectiveness of interlocking nails is undeniable. Yet, the techniques used must be continuously refined. Each surgery provides valuable insights for future improvements.
When repairing humeral fractures, proper insertion of interlocking nails is critical. Begin with a thorough assessment of the fracture type and patient’s anatomy. Position the patient appropriately on the surgical table. Ensure that you have clear access to the humerus. Mark the entry point carefully to avoid complications during insertion.
Next, prepare the surgical site with sterility in mind. Once ready, use a drill to create the entry site through the cortex. A guide wire must be inserted precisely to maintain alignment. Consider the angulation of the fracture for optimal nail placement. In some cases, this process may take longer. Patience is key; rushing can lead to misalignment or damaging surrounding tissues.
During the insertion, monitor the depth and trajectory closely. It may be tempting to push through quickly, but this often leads to errors. Use imaging techniques to guide your placement accurately. After securing the nail, check for stability. Sometimes, revision of technique might be needed. Reflect on the outcomes with each procedure. This step is vital for continuous improvement and skill refinement.
This bar chart illustrates the effectiveness of various humeral interlocking nail techniques based on their repair success rates. Each technique varies in success, with Technique B showing the highest rate at 90%.
Proper postoperative care is crucial after humeral interlocking nail surgery. Immediately following the procedure, patients need to focus on pain management. This often involves prescribed medications that should be taken as directed. Limiting certain movements is necessary to avoid stress on the healing bone.
Physical rehabilitation begins early, usually within days post-surgery. Gentle range-of-motion exercises can be introduced. These exercises are vital to prevent stiffness. Often, patients feel discouraged by their limitations. It’s essential to remember that gradual progress is normal. For some, simple tasks can feel overwhelming.
As healing advances, strengthening exercises become important. This helps restore muscle function. Patients should communicate with their healthcare provider about any discomfort. Reflection on progress is necessary. Recognizing small achievements can motivate continued effort. Building strength and confidence takes time, but each step is valuable in the recovery journey.
| Technique | Indications | Advantages | Postoperative Care | Rehabilitation |
|---|---|---|---|---|
| Intramedullary Nailing | Diaphyseal humerus fractures | Minimal soft tissue disruption, stable fixation | Pain management, wound care, monitoring for complications | Range of motion exercises, gradual weight bearing |
| Locking Plate Fixation | Proximal humeral fractures | Rigid stability, allows early mobilization | Elevation of arm, ice therapy, avoidance of heavy lifting | Physical therapy, strengthening exercises after 6 weeks |
| External Fixation | Complex fractures, soft tissue compromise | Preserves soft tissue, adjustable tension | Regular pin site care, avoiding wetting the fixator | Gradual introduction of movement, careful monitoring of alignment |
In humeral interlocking nail procedures, complications can arise, including infection, malalignment, and delayed union. According to a study in the Journal of Orthopedic Trauma, infection rates post-surgery can range from 3% to 12%. Precise surgical technique is critical to minimize these risks. Implementing strict aseptic protocols during the procedure can significantly lower infection rates.
Tips: Use a thorough sterilization process for all instruments. Consider preoperative antibiotics for patients with higher risk.
Malalignment is another concern, particularly if the nail isn’t properly aligned. This can lead to poor functional outcomes. Review by the Journal of Bone and Joint Surgery indicates that up to 25% of patients may experience malalignment without careful monitoring. Employing fluoroscopy during surgery helps ensure correct placement.
By keeping the communication open with your surgical team, you can swiftly address any emerging issues during the procedure. It’s vital to stay vigilant. Delayed union can occur if the fracture site is not adequately stabilized. Understanding the biomechanics of the humerus is essential to achieve optimal fixation.
Tips: Post-surgery, monitor for signs of delayed healing. Regular follow-ups can help catch complications early.